Abstract
Introduction: Zika virus has appeared in the Americas in the form of a major outbreak, and is now known to cause birth defects when pregnant women are infected. As a result, the Centers for Disease Control and Prevention issued travel guidelines, in the form of an elevational risk definition: destinations below 2000m are considered as at-risk.
Methods: We explored the distribution of known Zika virus vector mosquito species in relation to climatic conditions, elevation, latitude, and air traffic connections to the United States.
Results: In view of the tropical and subtropical nature of the mosquito species that are the primary Zika virus vectors, we point out that climate varies rather dramatically with respect to elevation and latitude, such that a single elevational criterion will be a poor predictor of potential for transmission.
Discussion: We suggest an initial adjustment would consider latitude in addition to elevation; a more definitive, quantitative analysis of risk would consider variables of ecology, climate, human condition, and connectivity of areas.
Funding Statement
Our work on this paper was not funded externally.Article
Zika virus is a flavivirus that is transmitted by aedine mosquito vectors, and that is showing a clear trend towards “emergence” in recent years1. The Centers for Disease Control and Prevention (CDC) recently (11 March 2016) issued guidelines for travel by pregnant women to Latin America, in light of the burgeoning Zika virus outbreak there2. The new guidelines advised a cut-off for risk, based strictly on elevation, with destinations below 2000 m considered as high-risk, and those above 2000 m considered as low-risk. In the Americas, among capitol cities, this recommendation would place only Mexico City, Quito (Ecuador), Bogotá (Colombia), and La Paz (Bolivia) in the low-risk category, and all others as high-risk.
However, we believe that simplicity in this case may come at the expense of clarity and good planning. As early as 1889, the concept of life zones had been proposed, which emphasizes the point that latitude mediates elevational trends3: elevations that are alpine at temperate latitudes will be forested and tropical at lower latitudes. Although, as CDC pointed out2, most occurrences of the primary vector—Aedes aegypti—are from below 2000 m, in a recent compilation, occurrences of the species above 2000 m were documented from Venezuela, Peru, Colombia, and Mexico4. A further concern is that ample evidence indicates that Zika virus can be transmitted by additional mosquito species beyond Ae. aegypti, with records from the previous range of the virus5,6,7, and emerging evidence of broader potential vector distribution in the Americas8; this revised view of Zika virus vector distribution would broaden the elevational (and geographic) range of potential transmission considerably.
Relationship between minimum temperature of the coldest month of the year9, elevation, and latitude. Black squares have a minimum temperature >20°; red squares are 15-20°; gray squares with a black outline are 10-15°, and light-gray squares are <10°.![Relationship between minimum temperature of the coldest month of the year [11], elevation, and latitude. Black squares have a minimum temperature >20°; red squares are 15-20°; gray squares with a black outline are 10-15°, and light-gray squares are <10°.](http://currents.plos.org/outbreaks/files/2016/04/Figure1_tropicalclimates-300x222.jpg)
Fig. 1: Relationship between elevation, latitude, and minimum temperature across the Americas.
Clearly, development of simple and clear guidelines for travel advice regarding Zika virus is desirable. However, as the CDC report acknowledged2, causal factors will be related to temperature and other environmental dimensions, and temperatures do not obey simple rules of elevational cutoffs—rather, elevation interacts with latitude in rather dramatic ways (see Figure 1), and even then many other factors act as one translates from macroclimate to microclimate, which is the factor of importance to populations of species10. Certainly, then, a simple elevational cutoff that applies equally in Bogotá and in Mexico City is not supported ecologically.
High-elevation travel destinations in the Americas are relatively few in number, with some (e.g., Quito and Bogotá) being equatorial, and others at higher latitude (e.g., La Paz). Hence, we believe that a more nuanced risk mapping that takes associated environmental variation into account would be markedly more effective. As commented by CDC2, more complex risk mapping efforts are possible, and preliminary maps have been published for Zika in the Americas11,12; these risk-mapping efforts should be extended and made more complete. In the short term, an improvement over a fixed-elevation criterion is to plot air destinations for US travelers in this latitude-elevation space (Figure 2): tropical-climate destinations can be identified rather easily, at least in a macrogeographic sense.
Destination airports for US travelers across the Americas (excluding the US and Canada, as Zika transmission is nil there, at least as of yet), derived from a recent risk-mapping effort focused on chikungunya virus in the Americas13, and plotted in an elevation-latitude space (see Figure 1). The largest circles indicate destinations with >100,000 passengers yearly; medium-sized circles 10,000-99,999 passengers yearly, and small circles <10,000 passengers yearly; gray squares indicate availability of conditions across the Americas (same data as shown in Figure 1).![Destination airports for US travelers across the Americas (excluding the US and Canada, as Zika transmission is nil there, at least as of yet), derived from a recent risk-mapping effort focused on chikungunya virus in the Americas [12], and plotted in an elevation-latitude space (see Figure 1). The largest circles indicate destinations with >100,000 passengers yearly; medium-sized circles 10,000-99,999 passengers yearly, and small circles <10,000 passengers yearly; gray squares indicate availability of conditions across the Americas (same data as shown in Figure 1).](http://currents.plos.org/outbreaks/files/2016/04/Figure2_destinationairports-300x222.jpg)
Fig. 2: Elevation-latitude relationships for destination airports across the Americas.
Relationship between minimum temperature of the coldest month of the year9, elevation, and latitude for destination airports across the Americas. Black squares have a minimum temperature >20°; red squares are 15-20°; gray squares with a black outline are 10-15°, and light-gray squares are <10°. Note the Bogotá, Colombia, airport, with an elevation above 2000 m and subtropical conditions.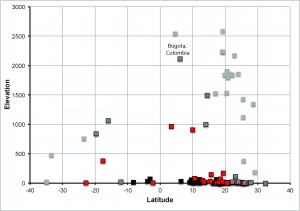
Fig. 3: Relationships between elevation, latitude, and minimum temperature for destination airports across the Americas.
We present this exploration not as a final analysis or set of recommendations, but rather as a suggestion to reconsider the too simple “elevational cutoff,” as it neglects the complex phenomena that drive disease transmission. The real-world translation of this concern is that travel to high-elevation Equatorial destinations is not at all without risk of Zika transmission, such that 2000 m is too low for those regions, whereas 2000 m will be too high for higher-latitude regions. At a minimum, travel guidelines should take into account the interaction between elevation and latitude; detailed climate data, suitability for key mosquito species, and information on mitigation efforts should be used to assemble a still-more-realistic approach for identifying risk areas for Zika virus transmission.
COMPETING INTERESTS
The authors have declared that no competing interests exist.
DATA AVAILABILITY STATEMENT
All data underlying the analyses presented in this publication are available at http://hdl.handle.net/1808/20727.
Acknowledgements
We thank our colleagues in disease-related studies at the University of Kansas and Mayo Clinic for their input into issues related to those treated in this contribution.References
- Zanluca C, Melo VCAd, Mosimann ALP, Santos GIVd, Santos CNDd, et al. (2015) First report of autochthonous transmission of Zika virus in Brazil. Memórias do Instituto Oswaldo Cruz 110: 569-572.
- Cetron M (2016) Revision to CDC’s Zika travel notices: Minimal likelihood for mosquito-borne Zika virus transmission at elevations above 2,000 meters. Morbidity and Mortality Weekly Report 65.
- Brown JH, Lomolino MV (1998) Biogeography. Massachusetts: Sinauer Associates.
- Kraemer MUG, Sinka ME, Duda KA, Mylne A, Shearer FM, et al. (2015) The global compendium of Aedes aegypti and Ae. albopictus occurrence. Scientific Data 2: 150035.
- Berthet N, Nakouné E, Kamgang B, Selekon B, Descorps-Declère S, et al. (2014) Molecular characterization of three Zika flaviviruses obtained from sylvatic mosquitoes in the Central African Republic. Vector-Borne and Zoonotic Diseases 14: 862-865.
- Diallo D, Sall AA, Diagne CT, Faye O, Faye O, et al. (2014) Zika virus emergence in mosquitoes in southeastern Senegal, 2011. PLoS ONE 9: e109442.
- Dick GWA, Haddow AJ (1952) Uganda S virus: A hitherto unrecorded virus isolated from mosquitoes in Uganda. (I) Isolation and pathogenicity. Transactions of the Royal Society of Tropical Medicine and Hygiene 46: 600-618.
- Pujhari S, Rasgon JL (2016) Zika virus: A newly emergent vector-borne public health threat in the Americas. PeerJ PrePrints 4:e1781v1781.
- Hijmans RJ, Cameron SE, Parra JL, Jones PG, Jarvis A (2005) Very high resolution interpolated climate surfaces for global land areas. International Journal of Climatology 25: 1965-1978.
- Kearney MR, Shamakhy A, Tingley R, Karoly DJ, Hoffmann AA, et al. (2014) Microclimate modelling at macro scales: A test of a general microclimate model integrated with gridded continental-scale soil and weather data. Methods in Ecology and Evolution 5: 273-286.
- Bogoch II, Brady OJ, Kraemer MU, German M, Creatore MI, et al. (2016) Anticipating the international spread of Zika virus from Brazil. Lancet 387: 335-336.
- Monaghan AJ, Morin CW, Steinhoff DF, Wilhelmi O, Hayden M, et al. (2016) On the seasonal occurrence and abundance of the Zika virus vector mosquito Aedes aegypti in the contiguous United States. PLoS Outbreaks. DOI: 10.1371/currents.outbreaks.50dfc7f46798675fc63e7d7da563da76.
- Escobar LE, Qiao H, Peterson AT (2016) Forecasting Chikungunya spread in the Americas via data-driven, empirical approaches. Parasites & Vectors 9: 112.

Leave a Comment
You must be logged in to post a comment.