Abstract
Background: In 2003, the Task Force on Quality Control of Disaster Management (WADEM) published guidelines for evaluation and research on health disaster management and recommended the development of a uniform data reporting tool. Standardized and complete reporting of data related to disaster medical response activities will facilitate the interpretation of results, comparisons between medical response systems and quality improvement in the management of disaster victims.
Methods: Over a two-year period, a group of 16 experts in the fields of research, education, ethics and operational aspects of disaster medical management from 8 countries carried out a consensus process based on a modified Delphi method and Utstein-style technique.
Results: The EMDM Academy Consensus Group produced an Utstein-style template for uniform data reporting of acute disaster medical response, including 15 data elements with indicators, that can be used for both research and quality improvement.
Conclusion: It is anticipated that the Utstein-style template will enable better and more accurate completion of reports on disaster medical response and contribute to further scientific evidence and knowledge related to disaster medical management in order to optimize medical response system interventions and to improve outcomes of disaster victims.
Funding Statement
This study was partially funded by grants from the EMDM, the Department of Emergency Medicine, University Hospital Brussels, the Research Group on Emergency and Disaster Medicine, Vrije Universiteit Brussel, and the Laerdal Foundation for Acute Medicine.Introduction
A significant limitation in research studies on the disaster medical management is the lack of standards for collecting and reporting data14. However, recent years have seen the publication of several guidelines for a common reporting structure2567. Nevertheless, the challenge of developing a rigorous and scientifically-based set of standardized data elements still remains. The availability of such data would enable researchers, educators and managers to study different aspects of the disaster medical response (DMR)8. To address this important issue, the Academy for Emergency Management and Disaster Medicine (EMDM Academy), an association comprised of research and education centres 9, initiated a project to establish a set of consensus-derived data elements using the well-documented Utstein-style method, including definitions and indicators for acute DMRs. Uniform Utstein-style reporting of data regarding out-of-hospital cardiac arrest, major trauma, and emergency medical dispatch, among others, has improved the international consensus on knowledge and practice in these areas101112. In line with other already published Utstein-style templates, the purpose of implementing a uniform reporting system of essential data, with respect to DMR, is to take advantage of the reporting system’s ability to conduct research, evaluation, training, and practice and quality improvement programs13. Therefore, there is a need for a set of measurable indicators which should define the key descriptors (data elements) that have impact on DMR, as well as the methods of measurement 1415. To date, the few metrics that exist have not yet been fully validated, nor have they universal acceptance 141516. This project proposes a set of data elements and indicators that can be used to uniformly collect and report on the data required to perform research and education related to the medical response in disaster situations.
Definition of Disaster
A review of the literature reveals the challenge that researchers and professionals face in having to agree on a generally accepted definition or conceptual interpretation of “disaster”. Over the years, books and entire journal issues have been dedicated to answer the question: “What is a disaster” 171819. Most of these definitions are valid in their respective context and reflect the authors’ opinions, as influenced by their disciplines or professional backgrounds12021222324.
The EMDM Academy Consensus Group – hereafter referred to as the Group – accepted from the outset that formulating a universally acceptable and all-encompassing definition of “disaster” was impossible. However, the Group was of the opinion that it was more important and feasible to identify, define and agree on the key characteristics that impact the DMR. This would allow for the development of a conceptual framework, which would better link these essential features. The Group also agreed that, from a DMR point of view, a disaster is an event in which the medical need exceeds the response capabilities in the affected area, mainly due to a large number and/or severity of injured or ill victims. This imbalance can be due to a quantitative and/or a qualitative shortage of resources (personnel and materials), but also to organizational or operational shortcomings. In this document, the word “disaster” is used as a synonym to “emergency” and “mass casualty incident/event”.
Methods
Inclusion/exclusion criteria
Disaster management is comprised of four stages or phases: mitigation, preparedness, response and recovery. This project does not include the mitigation, preparedness or the recovery functions, although we recognize that these activities have a role in influencing the implementation of an adequate DMR system. The consensus process for this study only addressed the acute DMR phase where the involvement of the healthcare professionals is recognized as having the greatest immediate impact on the outcome of the disaster casualties. Similarly, although public health interventions and mental health support can be part of the acute medical response, this study will only focus on the acute management of physically injured or ill patients, from the scene of the disaster to definitive treatment, otherwise known as the disaster acute medical care response.
The consensus process was conducted using the combination of a modified Delphi technique and the Utstein-style method, which is a modified nominal group technique2526.
The Consensus Group was composed of 20 people, represented eight countries and consisted of experts in the fields of research, education, ethics, and operational aspects of disaster medical management. Taking advantage of the two-week annual training session of the European Master in Disaster Medicine (EMDM)27, the Group first met in Novara (Italy) in June 2009 for many of them are also EMDM faculty members. The Group members represent the following organisations: the Disaster Medicine Section of the European Society for Emergency Medicine, the World Association for Disaster and Emergency Medicine, the World Health Organization, and the Academy for Emergency Management and Disaster Medicine.
During the first meeting, the Consensus Group decided that the main use for the data collected during a disaster would be to perform research and investigations of the acute medical care response in mass casualty incidents. It was determined that other aspects of the health response, such as public health, mental health and mass fatalities, would represent future projects.
The Consensus Group also defined the main factors which impact the acute DMR, i.e. the number, type and severity of the ill/injured survivors, time factors, environment factors, and the DMR system.
Subsequently, the Consensus Group, composed of the 16 authors, met in Brussels in March 2010 and was divided into four discussion subgroups in order to identify a list of potential data elements and indicators that would characterize the four main impact factors, based on the current disaster medical management and operations literature.
The third step consisted of a virtual modified Delphi technique using the virtual portal of the EMDM Academy and coordinated by the group leader (MD). The 16 group members were requested to indicate which data elements and indicators they considered essential for research and the evaluation of the acute medical response in disaster situations. The responses and their justifications were analysed and only those data elements and indicators which had been selected by at least 80% of the group members remained in the list. The remaining data elements and indicators were re-distributed to the Group members for a second round with the goal of reaching full consensus. Lack of comment was deemed implied agreement.
A final meeting with the 16 authors was organized at the Utstein Abbey, on the island of Mosterøy, off the Coast of Stavanger, Norway (23-25 November 2010). Utstein meetings are characterized by strong international collaboration and sponsorship of scientific organizations, using a process of gathering a number of experts in an isolated intellectual environment that engage in well-facilitated discussions. The employed consensus method is the “Utstein rotations” format, a modified nominal group technique. After an introductory session, the group is divided into four discussion panels, each of which are chaired by a moderator (ED, GR, AR, MD), and allocated to a fixed “station”. Such a subgroup meeting was governed by the following procedural format: the moderator briefly introduced the data elements to be discussed; then each member of the subgroup was asked to express his/her viewpoint on the subject; subsequently, the subgroup formed a statement that was representative of the opinion of the subgroup as a whole; after 90 minutes, the members of the subgroup moved to another “station”; with each incoming group, the moderator stated the conclusions of the previous group and subsequently, each member of the new subgroup was asked to express his/her opinion; this procedure was repeated, so that each participant was given the opportunity to contribute to each topic. The moderators then presented the overall conclusions of each “station” to the whole group, so that the remaining disagreements could be more widely debated. The final consensus on each data element and its indicators was then considered ratified if there was a complete absence of “nay” votes and rejected if one or more “nay” votes were recorded. All selected indicators were considered core data, i.e. data that should be collected.
A writing meeting was thereafter organized in Brussels in April 2011, followed by several e-meetings, until the time of publication.
Results
The data elements of the DMR including the indicators and metrics are listed in Table 1. The data regarding the pre-event settings and the disaster event description can be collected according to previous published guidelines, but should include at minimum the data listed in Tables 2 and 3 respectively.
Table 1. Disaster Acute Medical Response data elements and indicators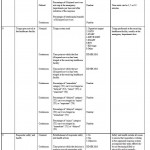
Table 2. Pre-event Setting
1. Population demographics
– Population size
– Age disaggregated
– Gender disaggregated
– Vulnerable groups
– Crude Mortality Rate (CMR)
– Under-5 Mortality Rate (U5MR)
– Endemic diseases – health profiles
3. Healthcare System (including capacities)
– Dispatch system
– EMS System
– Healthcare Facilities (primary, secondary, tertiary and specialty centers)
4. Disaster Medical Response System
– Medical Incident Management system including the different tiers (lines of authority)
– Criteria for activation of the disaster medical management plan (DMMP)
– Medical operations plan
– Concept of operations
– Medical information management
– Medical resources management
Table 3. Event Description
1. Type of Event
– Hazard type
– Warning
– Disaster scene (one or multiple)
– Duration (static or dynamic)
– Contagious or not
2. Impact intensity/magnitude
– Intensity scale
3. Impacted Area
– Location
– Surface
4. Subsequent related events
– Hazard type
– Warning
– Disaster scene (one or multiple)
– Duration (static or dynamic)
– Contagious or not
5. Time of onset
– DD/MM/YY HH:MM
– Day of the week
– Holiday
6. Environment
– Weather (temperature, humidity, precipitation type and amount, wind speed and direction)
– Height
7. Overall damage severity
– Score
8. Damage to infrastructure and life-sustaining services
– Potable water
– Sanitation
– Power (electricity)
– Energy relative to life sustainment
– Transportation
– Communication
– Fuel
9. Damage to healthcare system
– EMS System
– Healthcare Facilities (primary, secondary, tertiary) and Specialized Facilities
– Access to healthcare services
10. Casualties
– Age group (0-1 y, 1-17 y, 18-65 y, >65 y)
– Primary casualties
– Secondary casualties
– Casualty rate (number of ill/injured survivors / population exposed)
– Impacted (affected) population
– Severity of injuries (urgent versus non-urgent, hospitalized versus non-hospitalized, the ratio of immediate (T1) + delayed (T2) category survivors to the minimal (T3) category survivors
Event notification
In some events (transportation accidents, explosions) the impact will stretch or overwhelm the baseline of the actual healthcare system, however, this may not be readily apparent in other events, such as heat waves or epidemics. In addition, the initial recognition of the magnitude of the impact on the health system may be unclear even in obvious but widespread disasters28. Consequently, the event identification and notification could be immediate or delayed. According to the Group this can be measured by determining the interval between the time points of the disaster’s occurrence and the incoming call at the appropriate dispatch centre or equivalent in order to activate the medical response.
Activation of the disaster medical management plan (DMMP)
The activation of the DMMP and the subsequent notification of the appropriate medical functions should occur almost simultaneously. Notification consists of any process in which the appropriate medical functions and services are informed of a disaster situation that may require a response from those notified.
Any event that can cause a severe impact on routine healthcare services should be considered the threshold for the activation of the DMMP at the appropriate management tier in order to maximize the medical resources. Several trigger criteria for the activation of the DMMP, generally based on the total number of victims compared with system resources, the number of serious ill or injured survivors and/or loss of critical healthcare assets, are already in use28.
The Group proposes the following indicators to measure the effectiveness of the activation process of the DMMP:
Disaster medical operations coordination
Disaster management is the universal term meant to describe the structures and processes utilised to mitigate, prepare for, respond to and recover from, a disaster.
Disaster medical operations consist of all medical and non-medical actions required to achieve the response objectives following the activation of the DMMP.
The diverse organizations involved in the disaster response do not routinely function together, thus creating challenges in communication and coordination within the response system. Furthermore, disasters often involve activities across multiple levels of government2829.
Disaster medical operations coordination is the ability to respond to an event with health impacts by establishing a structure of supervision and organization consistent with the jurisdictional disaster management system and disaster medical management concept, principles and standards3031.
To perform the activities necessary to address the immediate and short-term health effects of a disaster, the health discipline must fall back on an integrated medical management system composed of an operating structure and response processes. The operating structure involves the division of tasks, including roles, responsibilities and authorities, as well as the coordination of diverse medical and non-medical operational assets. It is essential that these assets function together effectively towards minimizing mortality and morbidity of the disaster survivors. Rescue, decontamination, triage, stabilization, evacuation, and definitive treatment of disaster survivors, performed by all the involved operational assets, require integration through individual, mono- and/or multidisciplinary disaster management or coordination systems293132.
The response management activities include ad-hoc problem-solving, planning, decision making, communication, monitoring and evaluation33.
The main, ongoing, activities of medical operation coordination for an effective response include:
– maintaining situational awareness by continuous data collection and analysis. The data collected relates to the health impact, the health needs and available resources in and outside the affected area and the anticipated medical development of the disaster;
– medical communications and information management by establishing communication pathways between coordinating bodies and operational organizations, providing information to all stakeholders involved in the response, issuing progress reports at regular intervals, providing public information and interacting with the media;
– medical resource management by maintaining an inventory of available health resources (human and material), matching available health resources with defined needs and procuring and allocating health resources for unmet needs;
– management of the medical response by exercising authority to direct and control all aspects of the medical response by reaching consensus concerning goals and objectives of the response (medical response strategy) and the priorities for action (medical action plan). It also includes continuous monitoring in order to detect new problems and evaluate the effectiveness of the response activities and interventions, and providing quality assurance and control131.
To date, there has been limited research to identify, develop and validate indicators for measuring medical response management183435363737. In particular, the coordination process in the event of a disaster, due to the very nature of the operational and ethical constraints, has been the most challenging.
To fill this gap, the group developed a qualitative “Medical Operation Coordination Scale” in order to collect the required information on the performance of acute response actions or interventions in which coordination must be performed in a specific order to be effective (Appendix 1). Scoring of the effectiveness of the interventions is based on the method proposed by Parker et al208. For assessment purposes, “effectiveness” means that the action or intervention in question is both sufficient and timely enough so that the task to which it pertains can be accomplished. The scale is designed to provide an adequate number of categories to capture variation among ratings and allows for non-ratings through the “non applicable” and “not able to determine” response options, when appropriate. The scoring methodology and possible weighing of items on the Medical Operation Coordination Scale must await further validation through pilot-testing and field-testing.
The data required for measuring the effectiveness of the coordination of the DMR are focused on the essential health functions and management processes necessary to address the immediate and short-term health effects of a disaster at each level of the response. These include:
– On-scene initial actions including the assessment of the preliminary health effects;
– On-scene medical control and coordination including the development of a medical action plan;
– System-level medical coordination;
– Medical communication and information management; and
– Medical resource management.
Measuring the timeliness is fundamental because decision-making involving the mobilization of staff and other resources and establishing operational facilities and coordination centres are critical, ultimately affecting the time interval in which the survivors will receive their medical treatment.
In addition to speed, scale is also important. For dispensing medical care, throughput metrics enable calculation of the overall rate at which the ill/injured survivors will receive treatment.
Staff call-down is the ability to contact and mobilize staff to perform disaster response functions. For call-down, estimation metrics enable a count of the number of people who could be mobilized to medical management functions. Since the goal is to recruit staff for duty in a disaster, the calls must be conducted in a timely fashion, and the calls must reach all the necessary health personnel. In an actual disaster, the result should be that the response assets could be gathered at the time they are required. Consequently the “indicators” test the validity of the response system call-down lists and their ability to contact those staff in a timely matter: it estimates the percentage of staff who are able to report for duty to a given location at a certain time38.
The Group endorses the indicators proposed by Nelson et al38:
On-site triage
From a medical point of view, a disaster is characterized by the disproportion between the increased demand for medical response capacity and the actual medical resources available in order to manage the ill/injured survivors. This disparity can be due to a quantitative and/or qualitative shortage of human or physical resources as well as management problems. Therefore, it is imperative to set medical and organizational priorities. Due to prioritisation, not each individual victim will receive the optimal care immediately, and a certain selection of casualties is inevitable39.
Triage is often considered in narrow terms or as an isolated process, such as the categorization of casualties based on injury severity or the prioritization of patient treatment and/or transport39404142. Triage is a management tool meant to achieve the primary objectives of disaster medical management. It seeks to rapidly provide the greatest benefit for the largest number of casualties in order to minimize mortality, morbidity and indirect effects within the affected population and to re-establish as soon as possible the routine level of medical care. It also renders the delivery of medical care to an overwhelmed health system into a manageable task 394143343536373849.
The main factors that influence the triage process include the type and severity of the injuries/illnesses, the number of ill/injured survivors, the spatiotemporal distribution of the survivors, and the DMR system42505152535455.
1. The type and the severity of the injuries/illnesses according to the nature of the disaster: wounded, burned, blasted, intoxicated or contaminated victims, polytrauma patients, and casualties with combined injuries. The most important patients to identify are those critically ill or injured who will benefit immediately from the provision of resuscitative stabilization. Triage tools should identify which survivors are in need of immediate treatment as opposed to those whose treatment can be delayed and those who do not require medical treatment56.
2. The number of victims: the great majority of immediate disaster survivors are not critically injured or ill, as most lethal injuries or exposures kill immediately4525758. There is no simple method by which critically ill/injured survivors can be identified on the site of the disaster. This creates the potential for overtriaging to occur. However, in a recent study using the START system, 100% of “immediate category” survivors were identified in an actual disaster59. This is where triage can make its greatest impact in the acute medical response in managing the number of victims. The outcome of these “immediate category” survivors is a good indicator of the effectiveness of medical care in disasters526061.
3. The spatiotemporal distribution of the casualties:
4. The DMR system: triage management requires a tiered operational DMR system, which will define the extent and availability of resources425164. This requires effective coordination and information management within the entire DMR system414355616365.
It is well known that a short interval between the initial injury and definitive medical treatment offers the best chance of survival, shortens the period of convalescence and rehabilitation, and decreases functional disability66. Therefore, one of the most important tasks of the health sector is the setting-up of a well-organized evacuation system for the victims from the scene of the disaster to the appropriate healthcare facilities. Quick and accurate triage of the casualties at each level of the medical care chain is the cornerstone of the efficacy of such a system. At the scene of the disaster, triage is applied to determine mainly evacuation priorities. Appropriate distribution of patients among the available healthcare facilities reduces the burden to a manageable level and allows for the efficient use of resources. The triage process continues in hospitals but will be based on treatment priorities such as surgery and intensive care.
Consequently, the triage process must be seen in a wider context and is comprised of the following elements:
By fulfilling the aforementioned recommendations, disaster response activities will take place in a sequential and comprehensive fashion which minimizes patient care burden at each subsequent level of intervention and reduces the overall need for rationing care. As such, triage is one of the medical surge tools of the DMR system4267.
Triage is a progressive process. A primary (preliminary, early, swift, sweeping) survey that quickly reviews all victims should be in place. This survey would essentially determine the number of casualties, type and severity of injuries, and would identify those critically injured individuals who will immediately benefit from basic resuscitative procedures. Triage becomes more thorough and accurate, as the ill/injured survivors move along the lines of medical care and as the disproportion between the needs and available resources lessen6869. Triage is also a continuous process throughout the medical evacuation chain and is applied for as long as the disproportion between casualty demands and medical resources is ongoing. Primary triage is the first stage of patient triage, which usually occurs in the pre-hospital setting, but can occur in the emergency department for self-referred victims. Secondary triage is the re-evaluation of the patient’s condition after initial medical care and may occur at the scene, at an alternative medical treatment site, or at the hospital. Tertiary triage is the re-evaluation of a patient’s condition after further medical care and is ongoing during the patient’s stay in a healthcare facility. Thus, patients are continually reassessed at all levels of care throughout the entire journey of care435260707271 . Triage is also a dynamic process. To perform accurate triage, the following factors need to be considered: the nature, extent and severity of the injuries, the existence of associated or combined injuries, the mechanism of injuries, the prognosis, the change in the patient’s condition, the effectiveness of the treatment, the age of the patient, the number of patients, and cultural and religious factors4446607374. The triage decision process is additionally complex in disasters when following factors must be taken into consideration: effects of the disaster, location and accessibility of casualties, hostile environmental conditions, delay in treatment, limited resources in manpower, material, transportation means, distances to hospitals and treatment capacities of the receiving healthcare facilities 436073757676.
Being a progressive, continuous and dynamic and process, the triage category allocated to each injured/ill is adjusted as appropriate, and no triage decision should be considered final for as long as the disaster situation is ongoing69.
The accuracy of triage decisions may be an important factor in the effectiveness of the medical response and erroneous decisions may potentially compromise the clinical outcomes5261. Undertriaging in disasters is defined as the inappropriate assignment of “immediate category” survivors to receive delayed or minimal care. Overtriaging in disasters is defined as the inappropriate assignment of “delayed category” and “minimal category” survivors to receive immediate care. To date, only one triage system (START triage) has been retrospectively validated under disaster operational conditions59.
Further research is necessary to:
The Group proposes the following indicators of the triage process:
On-site medical care
The response to a disaster is time-sensitive and requires rapid intervention by healthcare providers in order to minimise death and morbidity858687.
Activities at the disaster scene include the collection, medical treatment and transport of the ill/injured survivors. The collection process includes victim location, primary triage and retrieval of the ill/injured survivors from the direct hazard impact area(s) and transfer into the formal system for evacuation to definitive care. This transfer may involve either holding the victims in one or more areas for on-site medical care or direct transfer to healthcare facilities. The medical treatment and transport process is comprised of:
Data relating to the triage and distribution/transportation of ill/injured survivors are handled as separate data elements.
For all victims, it is important to weigh the need for pre-hospital interventions against the need for prompt transport to the healthcare facility88. A pre-hospital time interval of greater than 60 minutes (the so-called “golden hour”89 is traditionally associated with a significant increase in the risk of death for severely injured patients90. However, this 60 minute cut-off point has no scientific basis88. Recent studies have concluded that there are no “golden” timelines91 and that there was no significant association between time and mortality for any EMS time interval (activation, response, on-scene, transport and total pre-hospital interval)929394.
Furthermore, the pre-hospital care of trauma patients is surrounded by much controversy889596. There is growing evidence questioning the benefit of specific advanced interventions for the pre-hospital management of severely injured patients94979899100. Advanced interventions may reduce morbidity or mortality in disasters with a large number of ill/injured survivors, in disasters possessing environmental obstacles, and in situations where the capacity of the healthcare system is temporarily overwhelmed, the means of evacuation are insufficient or the time for evacuation is prolonged747688101. The following advanced interventions may influence victim outcome:
Unfortunately, the implementation of advanced interventions in disaster situations or even in pre-hospital trauma care in rural areas has still to be scientifically validated6188. Furthermore, we do not know whether the health outcome of the disaster survivors is improved if the response is led by trained doctors as compared to trained emergency medical technicians102.
The Group proposes the following indicator to measure the effectiveness of the on-site medical care process:
Scene casualty clearance
There are several approaches for managing a disaster scene. Some authors associate scene organization with the goal of rapid transport and limited pre-hospital medical interventions (“scoop-and-run”). Others emphasize more extensive field medical interventions prior to transport (“stay-and-play”). The differences of opinion on this controversial issue (of stay-and-play versus scoop-and-run) could perhaps be harmonized by a “scoop-treat-and-run (SCOOTER)” system. This means that evacuation of the survivors should begin as soon as possible and that stabilization measures should be performed once the patient transport to the healthcare facility has started61101. It is likely that in a rural area the patient transfer may take longer. Therefore, on-scene stabilization may be advisable prior to transport to the appropriate hospital7476101.
The Group proposes the following indicators to measure scene casualty clearance:
Distribution of ill/injured survivors
Distribution of ill/injured survivors of disasters consists of best matching their medical needs to the available facilities, specialities, and admission capacities of healthcare facilities and the transportation modalities that accomplish the movement of victims to those healthcare facilities85.
Transportation of ill/injured survivors should start as soon as possible, according to the severity of illnesses or injuries, readiness of victims to evacuate and the availability of transportation means. Transportation assets have to match the needs of victims. Adequately trained and equipped healthcare providers should be available to care for seriously ill/injured survivors, while minor cases should be transported by any means possible, as long as they are approved by the officer in charge of the site85101.
Research observations indicate that a substantial number of disaster survivors, including severely injured patients, are transported to healthcare facilities by means other than an ambulance102103104105106107. In spite of this, research does not show whether disaster survivors benefit or suffer from rapid non-EMS transport compared with perhaps a more delayed but dedicated EMS ambulance transport.
Many studies on disasters have shown that it is common to witness a disproportionate number of survivors being transported from the scene to the closest healthcare facility57103104105108. In addition, self-transported survivors are also expected to present to the closest or most familiar healthcare facility61102.
Disasters can occur anywhere, and can affect metropolitan areas, containing one or more level-1 trauma centres, to remote areas, that do not have access to a nearby healthcare facility or to a fully equipped hospital109. These remote areas may have limited EMS capabilities, which further complicate the casualty disposition process106110. During incidents in which the needs of the ill/injured survivors outweigh the definitive care capacities of the receiving healthcare facility or when a prolonged, ongoing patient flow is expected, one healthcare facility can function as an “evacuation hospital”. This would involve receiving and stabilizing the disaster survivors and secondary distribution of all or part of those patients requiring further care to other facilities, depending on the patient load and local treatment capacity62101109111112113.
Maldistribution of ill/injured survivors in disasters is a recurring problem, as it overwhelms individual healthcare facilities and may not ensure optimal medical care103104108114115116117118119. The standard doctrine stipulates that victims should be transported to the most appropriate facilities. Several factors must be considered regarding the distribution and optimal use of hospital resources including the following:
In a study of 33 terror-related MCIs, Einav et al showed that the majority of all survivors and patients in urgent care were evacuated to the nearest hospitals and not necessarily to trauma centres, even in large urban regions112. They suggest that critically and mortally ill/injured survivors should be immediately evacuated to the nearest healthcare facility for primary resuscitation and stabilization (evacuation hospital concept), and that all other casualties should be evacuated to all other healthcare facilities in the area to avoid overwhelming any one hospital112. Other authors disagree with the concept of transporting the critically injured victims to the nearest hospital as it contradicts demonstrated improved outcomes achieved by trauma centres119120121122123.
Overcrowding or underutilisation of the available healthcare facilities can occur if patient distribution is not judiciously planned and executed119124. Effective coordination and communications are of critical importance in the distribution of disaster victims61101102109112.
The Group proposes the following indicators for assessing the distribution process of disaster victims:
Triage at the healthcare facility
Pre-hospital triage is not guaranteed, considering that disaster survivors can arrive to healthcare facilities via a number of transportation modes125126. Currently used emergency department triage scales, aiming to optimize the evaluation and treatment time of patients, according to the severity of their medical condition, may not be adequate for characterizing the nature and severity of the disaster surge127128. There is insufficient scientific evidence which positively correlates emergency department triage scales with predicted outcomes, and the same applies to disaster triage tools80129130.
Severely injured patients are not necessarily the first to arrive and may continue to arrive to the hospital for an extended, and often unknown, period of time131.
Some authors suggest that the sorting of incoming patients should be based both on the urgency of the treatment need and the anticipated utilization of important but scarce resources (resuscitation rooms, operating rooms, ICUs, medical imaging facilities). They proposed a simplified triage scheme with only 2 categories, i.e., all patients needing immediate interventions will be selected as priority, while all others will be assigned to the delayed care category, so long as their illnesses/injuries do not progress43130131132133.
The Group proposes the following indicators for the emergency department triage process:
Responder safety and health
Safety and health include all measures that ensure responders working in the organized response system can accomplish their tasks effectively without experiencing any physical or mental harm (130). First responders and hospital staff may be exposed to various environmental hazards during response operations, making them a significant liability to other victims and staff134135136137138. Furthermore, reports indicate that employees are less willing to report to duty during biological, chemical or radiation events, if they perceive a high degree of risk to themselves or their families139.
The Group proposes the following indicators that concern the safety and health of first responders and hospital staff:
Deactivation of operational plan.
Demobilization refers to activities that focus on the rapid return of the stood-down medical response resources to their normal function85. Demobilization of individual assets may occur at widely varying times, as increased workload of individual facilities may last several days28. Other important activities of the demobilization process, besides re-establishment of normal EMS operations and the rescheduling of regular staffing and normal activities of the healthcare facility, include addressing staff rehabilitation and health concerns, completing and securing incident documentation, conducting incident debriefing and review, and performance evaluation130.
When studying the potential benefit of disaster response systems, the cost of providing a response, measured in terms of time that health professionals are absent from their usual duties, may be an important consideration.
Therefore, the Group proposes as indicators:
Continuity of care for non-disaster-related ill and injured patients
It is likely that due to the increased load of disaster victims, a disruption of the normal activities of the pre-hospital and hospital services will occur134140. Therefore, the utilization of resources must be balanced with the need to maintain enough capacity to meet other local non-incident-related demands for medical care61.
The Group proposes the following indicators for the measurement of the continuity of care for non-disaster-related ill and injured patients:
Emergency department (ED) resource utilization
As the link between pre-hospital medical operations and in-hospital definitive treatment, emergency departments hold an important position in the care process of ill/injured disaster survivors127. Available data suggests that emergency departments are the access points for health care in sudden impact disasters4116141142, and that the majority of survivors are low-acuity patients who are discharged from the ED the same day462102104124143.
A hospital’s first notification of a disaster may often come with the first arriving victims, rather than from authorities in the field. Moreover, immediate information and updates about incoming victims are often insufficient or lacking102103144. The time it takes the first ill/injured survivor to arrive to the ED in a sudden impact disaster varies and can range from a few minutes to 30 minutes102104124143. In the majority of sudden impact disasters, the first peak of presentations occurs between 60 and 90 minutes, and most patients will have presented within 2 to 4 hours after the impact67143145146. In other sudden impact disasters like earthquakes, however, it may take several days before the ED volume returns to normal140147148.
The time interval from the onset of a disaster to the arrival of the first ill/injured survivor helps define the speed with which such incidents impact the EDs116. Factors likely to affect this time interval include hospital proximity, the ability of ill/injured survivors to transport themselves or be transported to EDs independent of the EMS system, and the prevalent traffic conditions102116149. The time of arrival of the last ill/injured survivor to the ED helps define the duration of the impact on the EDs116. Factors likely to influence this time interval are complex and include the hazard characteristics that affect the timeliness of search and rescue or evacuation, the number of victims, the pre-hospital response capacities, the effectiveness of casualty distribution and hospital proximity116. Appropriate ED response planning takes into account the time delay between the hazard impact and the first patient presentation, as well as the duration of patient influx116.
The “Emergency Department Time Interval” has been defined as the time lapse between ED triage to the time point of actual admission to the hospital150116. There is evidence suggesting that longer delays between the transfers from ED to ICU are linked to an increased mortality rate151.
Another important parameter of the health facility response is the rate at which ill/injured survivors arrive and use available resources. This rate is neither constant nor linear67104116131152153154). The ED influx of ill/injured survivors is not uniformly distributed over the duration of the medical response and treatment areas, such as ED, OR and ICU67. Estimations of surge by averaging patient numbers over the duration of the incident will underestimate the actual maximum surge rate67.
It is recommended to institute a unidirectional patient flow so that patient movement is uninterrupted, orderly and traceable. Patients will not be readmitted to the ED as their bed will likely be occupied by the next incoming casualty29101132155.
Another indicator of ED utilization is the critical surge to capacity ratio (ratio of “immediate category” patients to available resuscitation bays/rooms and teams), as it seems to have an impact on the mortality of “immediate category” injured survivors and as it has the potential to standardize the assessment of the ED capacity across disasters of varying size67155156157158. The increase of ED utilization or surge capacity in disasters is assessed by evaluating the ED treatment capacity in routine situations and after activation of the hospital disaster plan159.
The Group proposes the following indicators for the measuring of the utilization rate of emergency department resources:
Hospital resources utilization
Data concerning the utilization rate of operation rooms (OR), medical imaging, and intensive care units (ICU) should be collected, as these resources may be rate-limiting factors in the management of disaster survivors160.
The number of operating rooms may be a limiting factor in a high casualty load114. Current protocols advocate that only those casualties with life-threatening surgical conditions should be transferred to the operating rooms during the initial phase of victim influx67125161) and that only damage control resuscitation and surgery is performed at this stage 67161162163. The Group proposes the following indicators for measuring the utilization rate of the operating rooms:
Published reports from terrorist bombings noted that between 45% and 81% of injured survivors required plain radiology, 78% to 90% required computed tomography, and 12% to 38% required ultrasound sonography67104164165166167. Fast and accurate imaging including radiography, computed tomography and ultrasonography are used to help determine which ill/injured patient will be triaged to immediate surgery or an ICU168. With the exception of ultrasonography, which has proven to be an effective screening tool in disasters132161169170, no uniform policies exist with respect to the use of radiography and computed tomography in the initial phase of ill/injured survivors influx117131132161168170.
The Group proposes the following indicators for measuring the utilization rate of medical imaging modalities: the number of “immediate” and “delayed” survivors admitted to the ED, requiring medical imaging at 30 minutes intervals after initiation of the response, categorized by imaging technique (plain radiography, computed tomography, ultrasonography).
Disasters such as major chemical incidents, earthquakes, tsunamis, terrorist bombings and industrial explosions or pandemics can generate a large number of victims with critical clinical conditions requiring intensive care171172173174175. The intensive care surge demands may need to be sustained from days to weeks, in comparison to emergency department response, that typically only last a limited number of hours to days67155171. It is likely that the need for a rapid expansion of the ICU capacity in a mass casualty will prove extremely challenging171177178. Due to insufficient critical care staff, medical equipment and ICU space, the provision of a timely, high-quality critical care to a surge of critically ill or injured patients will prove difficult in many countries178179180181. In addition, ventilator availability may be another potential bottleneck as there are few acceptable alternatives152181183182. The Group proposes the following indicators for measuring the utilization rate of ICUs:
Outcome indicators
Currently, only one study provides evidence of a poorer outcome for surge patients originating from actual disasters than for routine trauma casualties that typically present one case at a time184.
Disasters, depending on their type and magnitude, result in various levels of morbidity and mortality. Most healthcare providers agree that the aim of the DMR is to “save as many lives as possible”, but no consensus exists as to what exactly constitutes a disaster or on how to deliver medical care to achieve this goal7172101185186187188189. Further research is required to investigate the ill/injured survivors’ outcomes with respect to DMR both in the pre-hospital and in-hospital phase. Factors such as the type of hazard or injury mechanism, field and ED triage, ill/injured survivors’ (peak) loads, speed of evacuation, distribution of victims to healthcare facilities, alterations in care, organizational issues, and education and training in disaster medical management of healthcare providers should be investigated80101114156184189190191.
We propose the following indicators for measuring morbidity:
Mortality rates are indicators of the magnitude of the disasters and its overall burden on the community. Rates of deaths, also termed mortality rates, may be more indicative than absolute numbers of deaths116. Several factors are likely to affect mortality rates in disasters, including hazard characteristics which in turn will affect illness/injury type and severity, the timeliness of the medical response, the casualty load, and the capacity and quality of medical care on the scene, in the ED and in the healthcare facility116.
The time interval between the onset of the illness or injury to definitive care is an important prognostic factor that can affect survivor outcome29161. Reports from past disasters have indicated a direct correlation between the time interval from rescue to definitive care and survivor mortality29126141161192193194195.
In assessing the effectiveness of DMR, we need to distinguish between the immediate deaths due to the hazard impact and the number of deaths that could have been potentially prevented, if ill/injured survivors were provided with timely medical attention, e.g. pre-hospital deaths, in-hospital deaths and “immediate” category deaths67. The overall mortality rate in disasters is skewed by the large number of the non-severely injured. The mortality rate of the “immediate category” survivors may be a more useful indicator of the effectiveness of the DMR, and allows a more meaningful comparison of outcomes from different disasters67196. The Group suggests that further research efforts should focus on the impact of medical, organizational, structural and cultural differences among disaster medical response systems on the morbidity and mortality of disaster survivors.
The Group proposes the following indicators for measuring mortality:
General Discussion
Similar to other branches of medicine, disaster medicine must possess a scientific basis. To date, there is no evidence-based literature that clearly defines the best medical response principles, concepts, structure and processes in the disaster setting7191197. The DMR is only as good as the assumptions on which it is based. Many of these assumptions are incorrect and/or are not based on systematically collected evidence102103198. Much of what is currently known about DMR results from descriptive studies and expert opinion7102. These insights are important, but lack the impact and the extrapolation power of conclusions drawn from objective data. It is not always easy to draw general conclusions based on single-centre studies, as different outcomes have been used, inclusion criteria vary, and structural, organizational and cultural differences among medical response systems may further hinder this process199. However, there is an increasing awareness among the speciality for the need to collect data that supports valid, reproducible conclusions on the effectiveness of the DMR184.
A prerequisite to adopting any evidence-based approach to DMR is the need to assemble a body of evidence from the results of relevant empirical studies13197. In situations of emergency, the gathering of reliable and valid data will always be difficult, as most healthcare providers prioritize the deliverance of care to a large number of victims over the documentation of cases during this time4102104. Furthermore, much of the relevant data becomes less accessible over time. Thus, it is important to establish dedicated field research teams that can be mobilized quickly after the onset of the disaster. Much of the data published worldwide is found in non–peer-reviewed publications, in unpublished reports or appears in the “grey” literature of government agencies or academic institutions. These are difficult to access, particularly through electronic indexing services102.
Health professionals and researchers from a broad spectrum of disciplines and specialities, contribute to the knowledge base of disaster medicine science. Although multidisciplinarity can be a strength, it can also be a hindrance due to differences of training and professional backgrounds. Moreover, there is a large variety in the organization of the DMR, both within and between countries. Without a standardized framework for describing and reporting the features that impact DMR, it is very difficult to compare results of DMR evaluations, and even more difficult to identify best practices25678. The lack of a common language also hinders intra- and interdisciplinary collaborations and appropriate training. Although there is seldom full agreement on all concepts in a particular field, it is counterproductive to have multiple, inconsistent and contradictory usages of many key terms. Unfortunately we found that this would describe the current situation in the disaster medicine discipline.
It is recognized that the study of DMR is a relatively new field. Developing a set of data elements, characterizing the medical response, and their indicators, based on research evidence, is in early stages. The identification and use of relevant indicators is a crucial part of determining the impact of interventions in DMR. The literature generally distinguishes between process or performance indicators and impact or outcome indicators. Performance indicators concern both the output of activities or interventions conducted and the process of implementation of the interventions. Outcome indicators are measures of the actual achievements intended, in our case, by the DMR. Mortality and morbidity rates are the most commonly used outcome indicators for medical management 115. The existing indicators, which have emerged through professional consensus, are not generally accepted and agreed on7. Without indicators that are measuring a DMR in a reliable and valid manner, it will not be possible to perform comparisons across different DMR systems, nor to evaluate the impact of response interventions, or to analyse the results in a scientific way. The Group trusts that the development of the indicators included in this Utstein-style template will serve as a framework for assessing the effectiveness of the DMR in the future. Moreover, collection of consistent data could lead, over time, to the development of a consensus on, and validation of, evidence-based process and outcome indicators.
The Group is mindful of the potential implementation difficulties that relate to Utstein-style templates11200201 . To address this concern, the template developed in this project will be made widely available by dissemination by the EMDM Academy, the research centres affiliated with the EMDM Academy, and the EMDM Alumni Association. To further facilitate implementation, a complete user manual and online template will be available for download free of charge at the respective websites.
The EMDM Academy Consensus Group encourages all readers to assist in the initial testing and immediate use of the template. Journal editors will be encouraged to adopt this Utstein-style template as reporting requirements for studies on DMR. These requirements will ensure consistent reporting of data and will allow reviewers and readers to accurately evaluate a study7.
Notwithstanding the fact that the vast majority of disasters occur in developing countries, peer reviewed publications on the effectiveness of the medical response to disasters in these countries are rare or not readily available202. Moreover, it is difficult to determine how applicable are research findings regarding DMR management, derived mostly from developed countries, to developing societies203. The Group hopes that this Utstein-style template for uniform reporting of acute DMR will encourage DMR research studies in developing countries.
The template needs to be field- and pilot-tested. Before formal pilot-testing, the template will require a more formative field-testing process. Such field tests are targeting the feasibility of using the tool and will provide feedback on the types of revisions that will improve its usability. Although the Utstein-style template can be used more easily for discrete scene disasters, it can be employed in large-scale events by collecting the data for each sector of the widespread scene. Similarly, data should be gathered for each individual healthcare facility and subsequently compiled, as appropriate. Formal pilot-testing would involve a greater number of disasters in order to provide a robust picture of the template’s performance across diverse types and scales of disasters. Currently, two studies are applying the template by using historical data from previous disasters and any modifications that will be deemed necessary will be incorporated as appropriate. The template is a dynamic document and will no doubt undergo a number of revisions as more data and experiences accumulate200. A follow-up meeting within two years will be held in order to revise the template and incorporate field studies, the experiences obtained with the first template, and any pertinent new research. However, the planned revision should not preclude the implementation of the current version of the template.
Databases available for DMR research are underdeveloped, incomplete and inaccurate13204205 . Although efforts have been made after the Asian tsunami to collect evidence by systematic reviews on a number of medical treatment interventions, no such studies have been performed concerning the effectiveness of disaster medical system interventions on the health outcomes of disaster survivors13206 . A uniform reporting method and template are essential in order to collect empirical data on DMR management. Such robust databases will allow DMR investigators to collect and interpret valid evidence that will impact disaster survivors’ outcomes13 . The EMDM Academy will provide the database infrastructure for the purpose of collecting, collating, and analysing data with respect to DMR and for facilitating multi-institutional research efforts in a standardized data set. Furthermore, individual data from disaster victims will also be collected in a specific database, i.e. VictimBase, an online victim library for medical professionals to create and share disaster victim profiles207 . Additionally, disaster victims from existing trauma or hospital registries should be earmarked so that data can easily be collected.
Conclusion
The present Utstein-style template is compiled by the EMDM Academy Consensus Group comprising of international representatives and provides a set of data elements for uniform reporting on the acute DMR. This will encourage more complete data collection as well as consistency in the reporting of findings and will enable comparison of research studies on medical response systems, both nationally and internationally. The data elements, definitions and indicators relating to the acute DMR identified in the present report will permit the collection of the most meaningful data, aggregate data analyses, and determination of the impact of different medical response strategies on outcome. This may contribute to further scientific evidence and knowledge related to acute DMR in order to optimize system interventions and to improve clinical outcomes of disaster survivors. This study on uniform reporting of acute medical response in disasters should be completed by data elements and indicators measuring the public health interventions and the mental health support.
Competing Interests
No competing interests exist.
Acknowledgements
The authors thank Myriam Plas, and Ase Henrichsen and Tore Laerdal for assistance in organizing the Group meetings in Brussels and the Utstein Abbey respectively. The authors thank Sergei Bankoul (SAMK), Tarig Bey (UCI), Yves Etienne (ICRC) and Kersten Gutschmidt (WHO) for their contribution at the first consensus meeting in Novara, Italy.Appendix 1
Medical Operation Coordination Scale
Item
Score
Notes
1.On-scene Initial Actions
First medical responder reports arrival on scene
0
1
2
3
4
N/A
N/D
First medical responder assumes role of medical incident commander
0
1
2
3
4
N/A
N/D
Protection of responders and victims
0
1
2
3
4
N/A
N/D
Preliminary assessment of the incident by first medical responder
0
1
2
3
4
N/A
N/D
First situation report to dispatch centre or equivalent by first medical responder
0
1
2
3
4
N/A
N/D
Request for appropriate additional personnel and non-personnel resources
0
1
2
3
4
N/A
N/D
Assignment of initial response roles on the scene of the incident
0
1
2
3
4
N/A
N/D
Total score
2.On-scene Medical Control and Coordination
Designated Incident Medical Commander (IMC) reports arrival at scene
0
1
2
3
4
N/A
N/D
Report of temporary IMC (first responder) to designated IMC
0
1
2
3
4
N/A
N/D
Establishing and operating of site-level medical command post
Medical assessment of the incident by IMC
0
1
2
3
4
N/A
N/D
Determining numbers/skill mix of personnel needed for optimal response to the incident (above and beyond those currently deployed)
0
1
2
3
4
N/A
N/D
Determining numbers/skill mix of personnel currently available for deployment
0
1
2
3
4
N/A
N/D
Determining non-personnel resources needed for optimal response to the incident (above and beyond those currently deployed)
0
1
2
3
4
N/A
N/D
Determining non-personnel resources currently available for deployment
0
1
2
3
4
N/A
N/D
Medical situation report(s) from IMC to Incident Commander
0
1
2
3
4
N/A
N/D
Medical situation report(s) from IMC to medical representative in Disaster Operational Centre (s)
0
1
2
3
4
N/A
N/D
Medical situation reports from IMC to medical healthcare facilities
0
1
2
3
4
N/A
N/D
Selection by IMC of areas to establish triage, treatment, distribution and transportation of ill/injured survivors, and a temporary morgue
0
1
2
3
4
N/A
N/D
Assignment by IMC of ancillary functions for medical response (search and rescue, triage, treatment, patient distribution, transportation, medical logistics, communications, morgue)
0
1
2
3
4
N/A
N/D
Establishment of an incident medical action plan by IMC
0
1
2
3
4
N/A
N/D
Situation reports from ancillary functions to IMC regarding status of incident
0
1
2
3
4
N/A
N/D
IMC briefing(s) to update medical command staff
0
1
2
3
4
N/A
N/D
Establishment of proper record keeping
0
1
2
3
4
N/A
N/D
Termination of medical field operations
0
1
2
3
4
N/A
N/D
Total score
3.System-level Medical Coordination
Notification of the assigned healthcare organization commander (EMS, hospitals, …)
0
1
2
3
4
N/A
N/D
Reporting of the assigned healthcare organization commander at appropriate location
0
1
2
3
4
N/A
N/D
Notification of the assigned on-scene medical commander
0
1
2
3
4
N/A
N/D
Reporting of the assigned medical commander at the incident command post
0
1
2
3
4
N/A
N/D
Notification of the assigned medical staff at local coordination centre
0
1
2
3
4
N/A
N/D
Reporting of designated medical staff at local coordination centre
0
1
2
3
4
N/A
N/D
Notification of the assigned medical staff at regional coordination centre
0
1
2
3
4
N/A
N/D
Reporting of the assigned medical staff at regional coordination centre
0
1
2
3
4
N/A
N/D
Notification of the assigned medical staff at federal coordination centre
0
1
2
3
4
N/A
N/D
Reporting of the assigned medical staff at federal coordination centre
0
1
2
3
4
N/A
N/D
Information flow between the different medical coordination tiers
0
1
2
3
4
N/A
N/D
Conducting operational after-action debriefing
0
1
2
3
4
N/A
N/D
Total score
4. Medical Communications and Information Management
Identification of intra- and interjurisdictional health/medical stakeholders to be incorporated into the information flow
0
1
2
3
4
N/A
N/D
Establishment of communication pathways between (medical) command, management locations and support agencies
0
1
2
3
4
N/A
N/D
Maintenance of continual connection with all parties involved throughout the incident management
0
1
2
3
4
N/A
N/D
Maintaining situational awareness using information gathered from medical stakeholders
0
1
2
3
4
N/A
N/D
Establishment of patient tracking procedures
0
1
2
3
4
N/A
N/D
Development and dissemination of information, alert or warnings to the public
0
1
2
3
4
N/A
N/D
Development and dissemination of information, alert, warnings or notifications to the incident managers and responders
0
1
2
3
4
N/A
N/D
Total score
5.Medical Resource Management
Mobilization of EMS healthcare personnel
0
1
2
3
4
N/A
N/D
Mobilization of medical facilities personnel
0
1
2
3
4
N/A
N/D
Mobilization of medical transportation means
0
1
2
3
4
N/A
N/D
Mobilization of medical equipment
0
1
2
3
4
N/A
N/D
Mobilization of medical supplies
0
1
2
3
4
N/A
N/D
Establishment of alternate care facilities
0
1
2
3
4
N/A
N/D
Assessment of resource requirements based on the evolving situation
0
1
2
3
4
N/A
N/D
Demobilization of resources
0
1
2
3
4
N/A
N/D
Total score
0 – Should have been done, but was not.
1 – Inadequate. The action or activity was started but was so incomplete or poorly performed as to be ineffective.
Did not function
2 – Somewhat adequate. The action or activity was started and was partially complete and/or performed in a partially effective manner.
Did function, but needs major improvement.
3 – Mostly adequate. The action or activity was performed in a generally effective and complete manner.
Did function, needs minor improvement.
4 – Completely adequate. The action or activity was completely performed in a fully effective manner.
Did function well.
N/A – Not applicable. The action or activity was not appropriate or necessary for this operation.
N/D – Not able to determine.
References
- TFQCDM/WADEM: Health Disaster Management: Guidelines for Evaluation and Research in the “Utstein Style”. Prehosp Disast Med 2003;17(Suppl 3):1-167.
- Lennquist S. Protocol for reports from major accidents and disasters. Int J Disast Med. 2004;2:57-64.
- Kohl PA, O'Rourke AP, Schmidman DL, Dopkin WA, Birnbaum ML. The Sumatra-Andaman Earthquake and Tsunami of 2004: The hazards, events, and damage. Prehosp Disaster Med. 2005;20:355-63.
- Stratton SJ, Tyler RD. Characteristics of medical surge capacity demand for sudden-impact disasters. Acad Emerg Med 2006;13:1193-1197.
- Leiba A, Schwartz D, Eran T, Blumenfeld A, Laor D, Goldberg A, Weiss G, Zalzman E, Ashkenazi I, Levi Y, Bar-Dayan Y. Disast-CIR: Disastrous incidents systematic analysis through components, interactions and results: Application to a large-scale train accident. J Emerg Med 2009;37:46-50.
- Kulling P, Birnbaum M, Murray V, Rockenschaub G. Guidelines for reports on health crises and critical health events. Prehosp Disast Med 2010;25:377-383.
- Bradt DA, Aitken P. Disaster medicine reporting: The need for new guidelines and the CONFIDE statement. Emergency Medicine Australasia 2010;22:483-487.
- Rüter A, Örtenwall P, Wikström T. Performance indicators for major incident medical management – a possible tool for quality control? Int J Disast Med 2004;2:52-55.
- Academy for Emergency Management and Disaster Medicine (EMDM Academy). www.emdmacademy.org
- Cummins RO, Chamberlain DA, Abramson NS, Allen M, Baskett PJ, Becker L, Bossaert L, Delooz HH, Dick WF, Eisenberg MS, Evans TR, Holmberg , Kerber R, Mullie A, Ornato JP, Sandoe E, Skulberg A, Tunstall-Pedoe H, Swanson R, Thies WH. Recommended guidelines for uniform reporting of data from out-of-hospital cardiac arrest: The Utstein style. A statement for health professionals from a Task Force of the American Heart Association, the European Resuscitation Council, the Heart and Stroke Foundation of Canada, and the Australian Resuscitation Council Circulation 1991;84:960-975
- Ringdal KG, CoatsTJ, Lefering R, Di Bartolomeo S, Steen PA, Røise O, Handolin L, Lossius HM and Utstein TCD expert panel. The Utstein template for uniform reporting of data following major trauma: A joint revision by SCANTEM, TARN, DGU-TR and RITG. Scand J Trauma Resusc Emerg Med 2008;16:7. doi:10.1186/1757-7241-16-7
- Castrén M, Karlsten R, Lippert F, Christensen EF, Bovim E, Kvam AM, Robertson-Steel I, Overton J, Kraft T, Engerstrom L, Garcia-Castrill Riego L, The Emergency Medical Dispatch expert group at the Utstein Consensus Symposium 2005. Recommended guidelines for reporting on emergency medical dispatch when conducting research in emergency medicine: The Utstein style. Resuscitation 2008;79:193-197.
- Kar-Purkayastha I, Clarke M, Murray V. Dealing with disaster databases – what can we learn from health and systematic reviews? PLoS Currents: Disasters 2011, Oct 7
- De Boer J, Debacker M. Quantifying medical disaster management. Int J Disast Med 2006;4:98-102
- Markenson D, Krug S. Developing pediatric emergency preparedness performance measures. Clinical Pediatric Emergency Medicine 2009;10:229-239.
- Lazar E, Cagliuso N, Gebbie K. Are we ready and how do we know? The urgent need for performance metrics in hospital emergency management. Disaster Med Public Health Preparedness 2009;3:57-60.
- Quarantelli EL (Guest Editor). What is a disaster? Six views of the problem. International Journal of Mass Emergencies and Disasters 1995;13:221‐364.
- Quarantelli EL (Editor). What is a disaster? Perspectives on the question. Routledge, London, 1998.
- Perry RW, Quarantelli EL (Editors). What is a disaster? New answers to old questions. International Research Committee on Disasters, Xlibris Corporation, 2005.
- Koenig KL, Dinerman N, Kuehl AE. Disaster nomenclature: A functional impact approach: The PICE System. Acad Emerg Med 1996; 3: 723–7.
- Al‐Madhari AF, Keller AZ. Review of disaster definitions. Prehosp Disast Med 1997;12:17‐21.
- Debacker M, Domres B, de Boer J. Glossary of new concepts in disaster medicine: A supplement to Gunn’s Multilingual Dictionary of Disaster Medicine. Prehosp Disast Med 1999;14:146-49.
- Nocera A. Australian major incident nomenclature: It may be a ‘disaster’ but in an ‘emergency’ it is just a mess. ANZ J Surg 2001;71:162-166.
- Shaluf IM, Ahmadun F, Said AM. A review of disaster and crisis. Disaster Prevention and Management 2003;12:24‐32.
- Linstone HA, Turoff M. The Delphi Method Techniques and Applications, 2002. https://is.njit.edu/pubs/delphibook/
- Delbecq AL, Van de Ven AH, Gustafson DH. Group Techniques for Program Planning: A Guide to Nominal Group and Delphi Processes, Green Briar Press,Middleton, 2004.
- European Master in Disaster Medicine (EMDM). www.dismedmaster.org
- Barbera JA, Macintyre AG. Medical surge capacity and capability: A management system for integrating medical and health resources during large-scale emergencies, Second Edition. U.S. Department of Health and Human Services, September 2007.
- O’Neill PA. The ABC’s of disaster response. Scand J Surg 2005;94:259-266.
- U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. Public health preparedness capabilities: National standards for state and local planning. March 2011.
- Peleg K, Kreiss Y, Ash N, Lipsky AM. Optimizing medical response to large-scale disasters: the ad hoc collaborative health care system. Ann Surg 2011;253:421-423.
- Frykberg ER. Disaster and mass casualty management: A commentary on the American College of Surgeons position statement. J Am Coll Surg 2003;197:857-859.
- Lusthaus C, Adrien MH, Anderson G, Carden F, Montalván GP. Organizational assessment: A framework for improving performance. International Development Research Centre and Inter-American Development Bank, 2002.
- Villarreal MS. Quality management tool for mass casualty emergency responses and disasters. Prehosp Disast Med 1997;12:200-209.
- de Boer J, van Remmen J. Order in Chaos. Modelling medical disaster management using emergometrics. Second revised edition. LiberChem Publication Solutions, Culemborg, The Netherlands, 2003.
- de Boer J, Debacker M. A more rational approach to medical disaster management applied retrospectively to the Enschede fireworks disaster, 13 May 2000. Eur J Emerg Med 2003;10:117-123.
- McCarthy ML, Brewster P, Hsu EB, Macintyre AG, MD, Kelen GD. Consensus and tools needed to measure health care emergency management capabilities. Disaster Med Public Health Preparedness 2009;3(Suppl 1):S45–S51.
- Nelson C, Chan EW, Fan C, Lotstein D, Caldarone LB, Shelton SR, Maletic AL, Parker AM, Felton A, Pomeroy A, Sloss EM. New tools for assessing state and local capabilities for countermeasure delivery. RAND Corporation, Technical Report 665, 2009.
- Debacker M. Disaster medicine. In Concepts and Developments in Emergency Medicine, Leuven, 1992
- Swan KG, Swan KG Jr. Triage: The past revisited. Milit Med 1996;161:448-452.
- Auf der Heide E. Disaster Response. Principles of preparation and coordination. St Louis, CV Mosby 1989:165-194.
- Bostick NA, Subbarao I, Burkle FM Jr, Hsu EB, Armstrong JH, James JJ. Disaster triage systems for large-scale catastrophic events. Disaster Med Public Health Preparedness 2008; 2(Suppl 1): S35-S39.
- Kennedy K, Aghababian RV, Gans L, Lewis CP. Triage: techniques and applications in decision making. Ann Emerg Med. 1996;28:136-144.
- Vayer JS, Ten Eyck P, Cowan ML. New concepts in triage. Ann Emerg Med 1986;15:927-930.
- Thomas JP. Les règles du triage des blessés. In : Dumas JM, Rufin JC (Eds) : Médicine de Catastrophe. Travaux du premier colloque national de médecine de catastrophe, Bordeaux 1983. Cerec 1984:87-95.
- Coupland RM, Parker PJ, Gray RC. Triage of war wounded: The experience of the International Committee of the Red Cross. Injury 1992;23:507-510
- Yeskey K. Sitting Ducks? While we cannot prepare for every possible contingency, EMS systems can maintain a heightened state of readiness for domestic and international terrorism. Emerg Med Serv 1996;25:61-64.
- Brennan RJ, Waeckerle A, Sharp TW. Chemical warfare agents: Emergency medical and emerging public health issues. Ann Emerg Med 1999;34:191-204.
- Kreiss Y, Merin O, Peleg K, Levy G, Vinker S, Sagi R, Abargel A, Bartal C, Lin G, Bar A, Bar-On E, Schwaber MJ, Ash N. Early disaster response in Haiti: the Israeli field hospital experience. Ann Intern Med. 2010;153:45-8.
- Noto R. La participation médicale à l’élaboration d’un plan de secours. IN : Dumas JM, Rufin JC (Eds) : Médecine de Catastrophe. Travaux du Premier Colloque National de Médecine de Catastrophe, Bordeaux 1983. Cerec 1984:32-46.
- Debacker M. Triage in case of disasters. In 7th International Training Course on Early Health Measures in Maxi-emergencies, CEMEC, San Marino, 1993:11-28.
- Frykberg ER. Triage: principles and practice. Scand J Surg 2005;94:272-278.
- Klein KR, Pepe PE, Burkle FM Jr, Nagel NE, Swienton RE. Evolving need for alternative triage management in public health emergencies: A hurricane Katrina case study. Disaster Med Public Health Preparedness 2008;2(Suppl1):S40-S44.
- Burkle FM Jr, Greenough PG. Impact of public health emergencies on modern disaster taxonomy, planning, and response. Disaster Med Public Health Preparedness 2008;2:192-199.
- Ryan JM. Triage: principles and pressures. Eur J Trauma Emerg Surg 2008;34:427-432.
- Kilner TM, Brace SJ, Cooke MW, Stallard N, Bleetman A, Perkins GD. In ‘big bang’ major incidents do triage tools accurately predict clinical priority?: A systematic review of the literature. Injury 2011;42:460-468.
- Centers for Disease Control and Prevention. Rapid assessment of injury among survivors of the terrorist attack on the World Trade Center – New York City, September 2001. MMWR 2002;51:1-5.
- Centers for Disease Control and Prevention. Epidemiologic assessment for illnesses and injuries after Hurricane Katrina – New Orleans, Louisiana, September 8-25, 2005. MMWR 2005;54:1018-21.
- Kahn CA, Schultz CH, Miller KT, Anderson CL. Does START triage work? An outcomes assessment after a disaster. Ann Emerg Med 2009;54:424-430.
- Waeckerle JF: Disaster planning and response. N Engl J Med 1991;324:815-821.
- Miller KT. Medical Services Scene Management. In Koenig KL, Schultz CH (Eds), Disaster Medicine: Comprehensive Principles and Practices. Cambridge University Press, New York, USA 2010:274-284.
- Leiba A, Blumenfeld A, Hourvitz A, Weiss G, Peres M, Laor D, Schwartz D, Arad J, Goldberg A, Levi Y, Bar-Dayan Y. Lessons learned from cross-border medical response to the terrorist bombings in Taba and Ras-el-Satan, Egypt, on 07 October 2004. Prehosp Disast Med 2005;20:253-257.
- Peleg K, Kellermann AL. Medical relief after earthquakes: It's time for a new paradigm. Ann Emerg Med 2011 Aug 18. doi:10.1016/j.annemergmed.2011.07.028.
- Burkle FM Jr. The triage dilemma: Opening Pandora’s box… ever so slowly. Critical care 2010;14:401.
- Burkle FM Jr, Hsu EB, Loehr M, Christian MD, Markenson D, Rubinson L, Archer FL. Definition and functions of health unified command and emergency operations centers for large-scale bioevent disasters within the existing ICS. Disaster Med Public Health Preparedness 2007;1:135-141.
- Pretto EA Jr, Safar P. National medical response to mass disasters in the United States. Are we prepared? JAMA 1991;266:47-50.
- Aylwin CJ, König TC, Brennan NW, Shirley PJ, Davies G, Walsh MS, Brohi K. Reduction in critical mortality in urban mass casualty incidents: analysis of triage, surge, and resource use after the London bombings on July 7, 2005. Lancet 2006;368:2219-2225.
- Slater MS, Trunkey DD. Terrorism in America. An evolving threat. Arch Surg 1997;132:1059-1066.
- Debacker M. Some considerations on triage in disasters. In: de Boer J, Dubouloz M (Eds), Handbook of Disaster Medicine, Zeist, The Netherlands, 2000: 329-335
- Ryan J, Gavalas M. What goes wrong at a disaster or major incident. Hosp Med 1998; 59:944-946.
- Institute of Medicine. Altevogt BM, Stroud C, Hanson SL, Hanfling DG, Gostin LO (Eds). Guidance for Establishing Crisis Standards of Care for Use in Disaster Situations: A Letter Report 2009. www.nap.edu/catalog/12749.html
- Ashkenazi I, Kessel B, Olsha O, Khashan T, Oren M, Haspel J, Ricardo A: Defining the problem, main objective, and strategies of medical management in mass-casualty incidents caused by terrorist events. Prehosp Disast Med 2008;23:82-89.
- Debacker M. Triage and regulation of mass burn casualties. Int Rev Armed Forces Med Serv 1992;65:135-140.
- Benson M, Koenig KL, Schultz CH. Disaster triage: START, then SAVE – A new method of dynamic triage for victims of a catastrophic earthquake. Prehosp Dis Med 1996;11:117-124.
- Llewellyn CH. Triage: In austere environments and echeloned medical systems. World J Surg 1992;16:904-909.
- Schultz CH, Koenig KL, Noji EK. A medical disaster response to reduce immediate mortality after an earthquake. N Engl J Med 1996;334:438-444.
- Garner A, Lee A, Harrison K, Schultz CH. Comparative analysis of multiple-casualty incident triage algorithms. Ann Emerg Med 2001;38:541-8.
- Cone DC, MacMillan DS. Mass-casualty triage systems: A hint of science. Acad Emerg Med 2005;12:739-741.
- Lerner EB, Schwartz RB, Coule PL, Weinstein ES, Cone DC, Hunt RC, Sasser SM, Liu JM, Nudell NG, Wedmore IS, Hammond J, Bulger EM, Salomone JP, Sanddal TL, Lord GC, Markenson D, O’Connor RE; Mass casualty triage: An evaluation of the data and development of a proposed national guideline. Disaster Med Public Health Preparedness 2008;2 (Suppl 1):S25-S34.
- Rothman RE, MD, Hsu EB, Kahn CA, Kelen GD. Research priorities for surge capacity. Acad Emerg Med 2006;13:1160-1168.
- Jenkins JL, McCarthy ML, Sauer LM, Green GB, Stuart S, Thomas TL, Hsu EB. Mass-casualty triage: Time for an evidence-based approach. Prehosp Disast Med 2008;23:3-8.
- Kahn CA, Lerner EB, Cone DC. Triage. In Koenig KL, Schultz CH (Eds), Disaster Medicine: Comprehensive Principles and Practices. Cambridge University Press, New York, USA 2010:174-183.
- Cone DC, Koenig KL. Mass casualty triage in the chemical, biological, radiological, or nuclear environment. Eur J Emerg Med 2005;12:287-302.
- Matzo M, Wilkinson A, Lynn J, Gatto M, Phillips S; Palliative care considerations in mass casualty events with scarce resources. Biosecurity and Bioterrorism: Biodefense Strategy, Practice, and Science 2009;7:199-210.
- Barbera J.A., Macintyre A.G. Medical and health incident management (MaHIM) system: A comprehensive functional system description for mass casualty medical and health incident management. Institute for Crisis, Disaster, and Risk Management, The George Washington University. Washington, D.C., October 2002.
- Target Capabilities List: A companion to the national preparedness guidelines. U.S. Department of Homeland Security. September 2007.
- Jackson BA, Faith KS, Willis HH. Evaluating the reliability of emergency response systems for large-scale incident operations. RAND Homeland Security and Defense Center, RAND Corporation Santa Monica, CA, USA, 2010.
- Liberman M, Roudsari BS. Prehospital trauma care: what do we really know? Curr Opin Crit Care 2007;13:691-696.
- Cowley RA. A total emergency medical system for the state of Maryland. Maryland State Med J 1975;24:37-45.
- Sampalis JS, Lavoie A, Williams JI, Mulder DS, Kalina M. Impact of on-site care, prehospital time, and level of in-hospital care on survival in severely injured patients. J Trauma 1993;34:252-261.
- Hoejenbos MJJ, McManus J, Hodgetts T. Is there one optimal medical treatment and evacuation chain for all situations: “Scoop-and-run” or “stay-and-play”. Prehosp Disast Med 2008;23(Suppl 2):s74-s78.
- Báez AA, Lane PL, Sorondo B, Giráldez EM. Predictive effect of out-of-hospital time in outcomes of severely injured young adult and elderly patients. Prehosp Disaster Med 2006; 21:427–430.
- Di Bartolomeo S, Valent F, Rosolen V, Sanson G, Nardi G, Cancellieri F, Barbone F. Are pre-hospital time and emergency department disposition time useful process indicators for trauma care in Italy? Injury 2007;38:305-311.
- Newgard CD, Schmicker RH, Hedges JR, Trickett JP, Davis DP, Bulger EM, Aufderheide T, Minei JP, Hata JS, Gubler KD, Brown TB, Yelle JD, Bardarson B, Nichol F and the Resuscitation Outcomes Consortium Investigators. Emergency Medical Services intervals and survival in trauma: Assessment of the “Golden Hour” in a North American prospective cohort. Ann Emerg Med 2010;55:235-246.
- Fowler R, Pepe PE. Prehospital care of the patient with major trauma. Emerg Med Clin N Am 2002;20:953-974.
- Blackwell T. Principles of emergency medical services systems. In: Marx JA, Hockberger RS, Walls RM, Adams JG, editors. Rosen’s Emergency medicine: concepts and clinical practice. St. Louis: Mosby 2002:2616–2625.
- Eckstein M, Chan L, Schneir A, Palmer R. Effect of prehospital advanced life support on outcomes of major trauma patients. J Trauma 2000;48:643-648
- Wang HE, Yealy DM. Out-of-hospital endotracheal intubation: where are we? Ann Emerg Med. 2006;47:532-541.
- Stiell IG, Nesbitt LP, Pickett W, Munkley D, Spaite DW, Banek J, Field B, Luinstra-Toohey L, Maloney J, Dreyer J, Lyver M, Campeau T, Wells GA, for the OPALS Study Group. The OPALS major trauma outcome study: impact of advanced life-support on survival and morbidity. CMAJ. 2008;178:1141-1152.
- Jayaraman S, Sethi D. Advanced trauma life support training for ambulance crews. Cochrane Database of Systematic Reviews 2010, Issue 1. DOI:10.1002/14651858.CD003109.pub2.
- Michaelson M, Hyams G, Blumenfeld A, Peleg K, Klein Y, Stein M, Poles L. Preparedness of health systems for mass casualty situations. A statement paper of guidelines aimed at building a structure of pre-hospital and hospital medical response to acts of terror. NATO Advanced Research Workshop on Mass Casualty Situations, Haifa, Israel, 10-15 April 2005.
- Auf der Heide E. The Importance of Evidence-Based Disaster Planning. Ann Emerg Med 2006;47:34-49.
- Quarantelli EL. Delivery of emergency medical care in disasters: Assumptions and realities. New York, NY: Irvington Publishers, Inc; 1983.
- Hogan DE, Waeckerle JF, Dire DJ, Lillibridge SR. Emergency department impact of the Oklahoma City terrorist bombing. Ann Emerg Med 1999;34:160-167.
- Okumura T, Takasu N, Ishimatsu S, Miyanoki S, Mitsuhashi A, Kumada K, Tanako K, Hinohara S. Report on 640 victims of the Tokyo subway sarin attack. Ann Emerg Med 1996;28:129–135.
- Bloch YH, Schwartz D, Pinkert M, Blumenfeld A, Avinoam S, Hevion G, Oren M, Goldberg A, Levi Y, Bar-Dayan Y. Distribution of casualties in a mass-casualty incident with three local hospitals in the periphery of a densily populated area: Lessons learned from the medical management of a terrorist attack. Prehosp Disast Med 2007;22:186-192.
- Hoyle JD Sr. Healthcare facility disaster management.In Koenig KL, Schultz CH (Eds), Disaster Medicine: Comprehensive Principles and Practices. Cambridge University Press, New York, USA 2010:285-311.
- Auf der Heide E. Disaster planning, part II: disaster problems, issues, and challenges identified in the research literature. Emerg Med Clin North Am 1996;14:453-481.
- Schwartz D, Pinkert M, Leiba A, Oren M, Haspel J, Levi Y, Goldberg A, Bar-Dayan Y. Significance of a level-2, “selective secondary evacuation” hospital during a peripheral town terrorist attack. Prehosp Disast Med 2007;22:59-66.
- Pinkert M, Lehavi O, Benin Goren O, Raiter Y, Shamis A, Priel Z, Schwartz D, Goldberg A, Levi Y, Bar-Dayan Y. Primary triage, evacuation priorities, and rapid primary distribution between adjacent hospitals – Lessons learned from a suicide bomber attack in downtown Tel-Aviv. Prehosp Disast Med 2008;23:337-341.
- Klausner JM, Rozin RR. The evacuation hospital in civilian disasters. Isr J Med Sci 1986;22:365-369.
- Einav S, Feigenberg Z, Weissman C, Zaichik D, Caspi G, Kotler D, Freund HR. Evacuation priorities in mass casualty terror-related events. Implications for contingency planning. Ann Surg 2004;239:304-310.
- Pinkert M, Leiba A, Zaltsman E, Erez O, Blumenfeld A, Avinoam S, Laor D, Schwartz D, Goldberg A, Levi Y, Bar-Dayan Y. The significance of a small, level-3 ‘semi evacuation’ hospital in a terrorist attack in a nearby town. Disasters 2007;31:227-235.
- Lennquist S. Management of major accidents and disasters: An important responsibility for the trauma surgeons. J Trauma 2007;62:1321-1329.
- Asaeda G. The day that the START Triage System came to a stop: observations from the World Trade Centre disaster. Acad Emerg Med 2002;9:255-256.
- Arnold J, Tsai M, Halpern P, Smithline H, Stok E, Ersoy G. Mass casualty, terrorist bombings—epidemiological outcomes resource utilisation and time-course of emergency needs (Part I). Prehosp Disast Med 2003;18:220-234.
- Halpern P, Tsai M, Arnold J, Stok E, Ersoy G. Mass casualty and terrorist bombings—implications for emergency departments and hospital emergency response (Part II). Prehosp Disast Med. 2003;18:235-241.
- Hoey B, Schwab C. Level I center triage and mass casualties. Clin Orthop Relat Res 2004;422:23-29.
- Zoraster RM, Chidester C,Koenig W. Field triage and patient maldistribution in a mass-casualty incident. Prehosp Disast Med 2007;22:224-229.
- Shapira SC, Adatto-Levi R, Avitzour M, Rivkind AI, Gertsenshtein I, Mintz Y. Mortality in terrorist attacks: A unique modal of temporal death distribution. World J Surg 2006;30:2071-2077.
- Leiba A, Halperin P, Kotler D, Blumenfeld A, Soter D, Weiss G, Peres M, Laor D, Levi Y, Goldberg A, Bae-Dayan Y. Lessons from a terrorist attack in Tel-Aviv market: Putting all the golden eggs in one basket might save lives. Int J Disast Med 2005;2:157-160.
- Rivara FP, MD, Nathens AB, Jurkovich GJ, Maier RV. Do trauma centers have the capacity to respond to disasters? J Trauma 2006;61:949-953.
- MacKenzie EJ, Rivara FP, Jurkovich G, Nathens AB, Frey KP, Egleston BL, Salkever DS, Scharfstein DO. A national evaluation of the effect of trauma center care on mortality. New Engl J Med 2006;354:366-378.
- Rodoplu U, Arnold JL, Tokyay R, Ersoy G, Cetiner S, Yucel T. Mass-casualty terrorist bombings in Istanbul, Turkey, November 2003: report of the events and the prehospital emergency response. Prehosp Disast Med 2004;19:133-145.
- Shamir MY, Weiss YG, Willner D, Mintz Y, Bloom AI, Weiss Y, Sprung CL, Weissman C. Multiple casualty terror events: The anesthesiologist’s perspective. Anesth Analg 2004;98:1746-1752.
- Biancolini CA, Del Bosco CG, Jorge MA. Argentine Jewish Community Institution bomb explosion. J Trauma 1999;47:728-732.
- McCarthy ML, Aronsky D, Kelen GD. The measurement of daily surge and its relevance to disaster preparedness. Acad Emerg Med 2006;13:1138-1141.
- Davidson SJ, Koenig KL, Cone DC. The daily flow of patients is not surge: “management is prediction”. Acad Emerg Med 2006;13:1095-1096.
- Farrohknia N, Castrén M, Ehrenberg A, Lind L, Oredsson S, Jonsson H, Asplund K, Göransson KE. Emergency department triage scales and their components: A systematic review of the scientific evidence. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2011;19:42.
- Emergency Management Principles and Practices for Healthcare Systems. The Institute for Crisis, Disaster, and Risk Management (ICDRM) at the George Washington University (GWU); for the Veterans Health Administration (VHA)/US Department of Veterans Affairs (VA). Washington, D.C., June 2006.
- Einav S, Aharonson-Daniel L, Weissman C, Freund HR, MD, Peleg K, and the Israel Trauma Group. In-hospital resource utilization during multiple casualty incidents. Ann Surg 2006;243:533-540.
- Kluger Y, Mayo A, Soffer D, Aladgem D, Halperin P. Functions and principles in the management of bombing mass casualty incidents: lessons learned at the Tel-Aviv Souraski Medical Center. Eur J Emerg Med 2004;11:329-334.
- Hirshberg A, Holcomb JB, Mattox KL. Hospital trauma care in multiple-casualty incidents: a critical review. Ann Emerg Med 2001;37:647-652.
- Okumura T, Suzuki K, Fukuda A, Kohama A, Takasu N, Ishimatsu S, Hinohara S. The Tokyo subway sarin attack: disaster management, Part 2: Hospital Response. Acad Emerg Med 1998;5:618-624.
- Centers for Disease Control and Prevention. Severe acute respiratory syndrome—Taiwan 2003. MMWR Weekly 2003;52:461-466.
- Berkowitz Z, Horton DK, Kaye WE. Hazardous substances releases causing fatalities and/or people transported to hospitals: rural/agricultural vs. other areas. Prehosp Disast Med 2004;19:213-220.
- Booth CM, Stewart TE: Severe acute respiratory syndrome and critical care medicine: The Toronto experience. Crit Care Med 2005;33:S53-S60
- Horton DK, Orr M, Tsongas T, Leiker R, Kapil V. Secondary contamination of medical personnel, equipment, and facilities resulting from hazardous materials events. Disaster Med Public Health Preparedness 2008;2:104-113.
- Qureshi K, Gershon RRM, Sherman MF, Straub T, Gebbie E, McCollum M, Erwin MJ, Morse SS. Health care workers’ ability and willingness to report to duty during catastrophic disasters. J Urban Health 2005;82:378-388.
- Roy N, Shah H, Patel V, Coughlin RR. The Gujarat earthquake (2001) experience in a seismically unprepared area: community hospital medical report. Prehosp Disast Med 2002;17:186-195.
- Mallonee S, Shariat S, Stennes G, Waxweiler R, Hogan D, Jordan F. Physical injuries and fatalities resulting from the Oklahoma City bombing. JAMA 1996;27:382-387.
- Arnold JL, Halpern P, Tsai MC, Smithline H. Mass casualty terrorist bombings: a comparison of outcomes by bombing type. Ann Emerg Med 2004;43:263-273.
- Leiba A, Ashkenasi I, Nakash G, Pelts R, Schwartz D, Goldberg A, Levi Y, Bar-Dayan Y. Response of Thai hospitals to the Tsunami disaster. Prehosp Disast Med 2006;21:s32-s37.
- Mohammed AB, Mann HA, Nawabi DH, Goodier DW, Ang SC. Impact of London’s terrorist attacks on a major trauma center in London. Prehosp Disast Med 2006;21:340-344.
- Okumura T, Suzuki K, Fukuda A, Kohama A, Takasu N, Ishimatsu S, Hinohara S. The Tokyo subway sarin attack: disaster management, part 1: community emergency response. Acad Emerg Med 1998;5:613-617.
- Cushman J, Pachter H, Beaton H. Two New York City hospitals’ surgical response to the September 11, 2001, terrorist attack in New York City. J Trauma 2003;54:147-155.
- Stratton SJ, Hastings VP, Isbell D, Celentano J, Ascarrunz M, Gunter CS, Betance J. The 1994 Northridge earthquake disaster response: the local emergency medical services agencies experience. Prehosp Disast Med 1996;11:172-179.
- Liang NJ, Shin YT, Shin FY, WU HM, Wang HJ, Shi SF, Liu MY, Wang BB; Disaster epidemiology and medical response in the Chi-Chi earthquake in Taiwan. Ann Emerg Med 2001;38:549-555.
- Stein M, Hirshberg A: Medical consequences of terrorism. Surg Clin North Am 1999;79:1537-1552.
- Bayram JD, Zuabi S, Subbarao I. Disaster metrics: quantitative benchmarking of hospital surge capacity in trauma-related multiple casualty events. Disaster Med Public Health Preparedness 2011;5:117-124.
- Clark K, Normile LB. Influence of time-to-interventions for emergencv department critical care patients on hospital mortality. J Emerg Nursing 2007;31:6-13.
- Singer AJ, Singer AH, Halperin P, Kaspi G, Assaf J. Medical lessons from terror attacks in Israel. J Emerg Med 2007;32:87-92.
- Hirshberg A, Bradford SG, Granchi T, Wall MJ, Mattox KL, Stein M. How does casualty load affect trauma care in urban bombing incidents? A quantitative analysis. J Trauma 2005;58:686-695.
- Karp E, Sebbag G, Peiser J, Dukhno O, Ovnat A, Levy I, Hyam E, Blumenfeld A, Kluger Y, Simon D, Shaked G. Mass casualty incident after the Taba terrorist attack: an organisational and medical challenge. Disasters 2007;31:104-112.
- Mahoney EJ, Harrington DT, Biffl WL, Metzger J, Oka T, Cioffi WG. Lessons learned from a nightclub fire: institutional disaster preparedness. J Trauma 2005;58:487-491.
- Hupert N, Hollingsworth E, Xiong W. Is overtriage associated with increased mortality? Insights from a simulation model of mass casualty trauma care. Disaster Med Public Health Preparedness. 2007;1(Suppl 1):S14-S24.
- Hirshberg A, Stein M, Walden R. Surgical resource utilization in urban terrorist bombings: a computer simulation. J Trauma 1999;47:545-550.
- Hirshberg A, Frykberg ER, Mattox KL, Stein M. Triage and trauma workload in mass casualty: A computer model. J Trauma 2010;69:1074-1082.
- Hirshberg A, Scott BG, Granchi T, Wall MJ Jr, Mattox KL, Stein M. How does casualty load affect trauma care in urban bombing incidents? A quantitative analysis. J Trauma 2005;58:686-695.
- Traub M, Bradt DA, Joseph AP. The surge capacity for people in emergencies (SCOPE) study in Australasian hospitals. MJA 2007;186:394-398.
- Frykberg ER. Medical management of disasters and mass casualties from terrorist bombings: how can we cope? J Trauma. 2002;53:201-212.
- Bashir MO, Abu-Zidan FM, Lennquist S: Will the damage control concept influence the principles for setting of priorities for severely traumatized patients in disaster situations? Int J Disast Med 2003;2:97-102.
- Almogy G, Belzberg H, Mintz Y, Pikarsky AK, Zamir G, Rivkind AI. Suicide bombing attacks: update and modifications to the protocol. Ann Surg 2004;239:295-303.
- Raja AS, Propper BW, VandenBerg SL, Matchette MW, Rasmussen TE, Johannigman JA, Davidson SB. Imaging utilization during multiple casualty incidents. J Trauma 2010;68:1421-1424.
- Benjaminov O, Sklair-Levy M, Rivkind A, Cohen M, Bar-Tal G, Stein M. Role of radiology in evaluation of terror attack victims. Am J Roentgenol 2006;187:609-616
- Beck-Razi N, Fischer D, Michaelson M, Engel A, Gaitini D. The utility of focused assessments with sonography for trauma as a triage tool in multiple-casualty incidents during the second Lebanon war. J Ultrasound Med 2007;26:1149-1156.
- Turegano-Fuentes F, Perez-Diaz D, Sanz-Sanchez M, Ortiz Alonso J. Overall assessment of the response to terrorist bombings in trains, Madrid, 11 March 2004. Eur J Trauma Emerg Surg 2008;34:433-441.
- Sosna J, Sella T, Shaham D, Shapira SC, Rivkind A, Bloom AI, Libson E. Facing the new threats of terrorism: Radiologists’ perspectives based on experience in Israel. Radiology 2005;237:28-36.
- Sarkisian AE, Khondkarian RA, Amirbekian NM, Bagdasarian NB,Khojayan RL, Oganesian YT. Sonographic screening of mass casualties for abdominal and renal injuries following the 1988 Armenian earthquake. J Trauma 1991;31:247-250.
- Körner M, Krötz MM, Wirth S, Huber-Wagner S, Kanz KG, Boehm HF, Reiser M, Linsenmaier U. Evaluation of a CT triage protocol for mass casualty incidents: results from two large-scale exercises. Eur Radiol 2009;19:1867-1874.
- Christian MD, Devereaux AV, Dichter JR, Geiling JA, Rubinson L. Definitive care for the critically ill during a disaster: Current capabilities and limitations: From a task force for mass critical care summit meeting, January 26-27, 2007, Chicago, IL. Chest 2008;133(Suppl 5):8S-17S.
- Baker DJ. Critical care requirements after mass toxic agent release. Crit Care Med 2005; 33(1 Suppl):S66-S74.
- Halpern P, Rosen B, Carasso S, et al. Intensive care in a field hospital in an urban disaster area: lessons from the August 1999 earthquake in Turkey. Crit Care Med 2003; 31:1410-1414.
- Sever MS, Vanholder R, Lameire N. Management of crush-related injuries after disasters. N Engl J Med 2006;354:1052-1063.
- Maegele M, Gregor S, Steinhausen E, Bouillon B, Heiss M, Perbix W, Wappler F, Rixen D, Geisen J, Berger-Schreck B, Schwartz R. The long distance tertiary air transfer and care of tsunami victims: injury pattern and microbiological and psychological aspects. Crit Care Med 2005;33:1136-1140.
- Arthurson G. The tragedy of San Juanico - the most severe LPG disaster in history. Burns 1987;13:87-102.
- Rubinson L, Nuzzo JB, Talmor DS, O’Toole T, Kramer BR, Inglesby TV: Augmentation of hospital critical care capacity after bioterrorist attacks or epidemics: recommendations of the Working Group on Emergency Mass Critical Care. Crit Care Med 2005;33:2393-2403.
- Kanter RK, Moran JR. Pediatric hospital and intensive care unit capacity in regional disasters: Expanding capacity by altering standards of care. Pediatrics 2007;119:94-100.
- Parker MM. Critical care and disaster management. Crit Care Med 2006;34(Suppl 3):S52-S55.
- Halpern NA, Pastores SM, Thaler HT, Greenstein RJ. Changes in critical care beds and occupancy in the United States 1985-2000: differences attributable to hospital size. Crit Care Med 2006;34:2105-2112.
- Hick JL, Rubinson L, O’Laughlin DT, Farmer JC. Clinical review: Allocating ventilators during large-scale disasters - problems, planning, and process. Critical Care 2007;11:217 (doi:10.1186/cc5929).
- Neyman G, Irvin CB: A single ventilator for multiple simulated patients to meet disaster surge. Acad Emerg Med 2006;13:1246-1249.
- Branson RD, Rubinson L: A single ventilator for multiple simulated patients to meet disaster surge (letter). Acad Emerg Med 2006;13:1352-1353.
- Peleg K, Rozenfeld M, Stein M. Poorer outcomes for mass casualty event victims: Is it evidenced based? J Trauma 2010;69:653-658.
- Ball CG, Kirkpatrick AW, Mulloy RH, Gmora S, Findlay C, Hameed SM. The impact of multiple casualty incidents on clinical outcomes. J Ttrauma 2006;61:1036-1039.
- Altered Standards of Care in Mass Casualty Events. Prepared by Health Systems Research Inc. under Contract No. 290-04-0010. AHRQ Publication No. 05-0043. Rockville, MD: Agency for Healthcare Research and Quality. April 2005.
- Koenig KL, Lim HCS, Tsai SH. Crisis standards of care: Refocusing health care goals during catastrophic disasters and emergencies. J Exp Clin Med 2011;3:159-165.
- Hick JL, Hanfling D, Cantrill SV. Allocating scarce resources in disasters: emergency department principles. Ann Emerg Med 2011 (in press). DOI:10:1016/j.annemergmed.2011.06.012.
- Shultz CH, Annas GJ. Altering the standards of care in disasters-Unnecessary and dangerous. Ann Emerg Med 2011 (in press). DOI:10.1016/j.annemergmed.2011.07.037.
- Altay N, Green WG III. OR/MS research in disaster operations management. European Journal of Operational Research 2006;175:475-493.
- Hubloue I, Debacker M. Education and research in disaster medicine and management: Inextricably bound up with each other. Eur J Emerg Med 2010;17:129-130.
- Fryberg ER, Tepas JJ, Alexander RH: The 1983 Beirut airport terrorist bombing: injury patterns and implications for disaster management. Am Surg 1989;55:134-141.
- Brismar B, Bergenwald L: The terrorist explosion in Bologna Italy 1980: an analysis of the efforts and injuries sustained. J Trauma 1982;22:216-220.
- Rignault DP, Deligny MC: The 1986 terrorist bombing experience in Paris. Ann Surg 1989;209:368-373.
- Feliciano DV, Anderson GV, Rozycki GS, Ingram WK, Ansley JP, Namias N, Salomone JP, Cantwell JD: Management of casualties from the bombing at the centennial Olympics. Am J Surg 1998;176:538-543.
- Frykberg ER. Principles of Mass Casualty Management Following Terrorist Disasters. Ann Surg 2004;239:319-321
- Bradt DA. Evidence-based decision-making: Applications in disaster relief operations. Prehosp Disast Med 2009;24:479-492.
- Noji EK. Disasters: Introduction and state of the art. Epidemiol Rev2005;27:3-8.
- Jäderling G, Konrad D. Standardized process and outcome assessment tool. In De Vita MA et al (eds), Textbook of rapid response systems: Concepts and implementation. Springer NY, 2011:397-403.
- Sollid SJM, Lockey D, Lossius HM, Prehospital advanced airway management expert group. A consensus-based template for uniform reporting of data from pre-hospital advanced airway management. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine 2009;17:58.
- Cone DC, Jaslow DS, Brabson TA. Now that we have the Utstein Style, are we using it? Acad Med Emerg 1999;6:923-928.
- Roy N, Thakkar P, Shah H. Developing-world disaster research: Present evidence and future priorities. Disaster Med Public Health Preparedness 2011;5:112-116.
- Quarantelli EL. Ten criteria for evaluating the management of community disasters. Preliminary paper #241. Disaster Research Center, University of Delaware, 1996.
- Guha-Sapir D, Below R. The quality and accuracy of disaster data. A comparative analysis of three global data sets. Provention Consortium, The Disaster Management Facility, The World Bank, 2002.
- Tschoegl L, Below R, Guha-Sapir D. An analytical review of selected data sets on natural disasters and impacts. CRED, March 2006.
- Clarke M; Evidence Aid – from the Asian tsunami to the Wenchuan earthquake. J Evid Based Med 2008;1:9-11. DOI: 10.1111/j.1756-5391.2008.00007.x
- VictimBase. www.victimbase.org.
- Parker A, Nelson C, Shelton SR, Dausey DJ, Lewis MW, Pomeroy A, Leuschner KJ. Measuring Crisis Decision Making for Public Health Emergencies. RAND Corporation, Technical Report 712, 2009.

Leave a Comment
You must be logged in to post a comment.